- Blog
- Spongebob squarepants season 1 episode 1 part 1
- Optixcam summit series software
- Vintage haro bicycle for sale
- Mount and blade warband campaign ai
- Toon boom harmony 17
- Suite adobe cs6 crack mac
- Automation studio p6 download free
- Digimon world 2 trade list
- Separation studio descargar
- Lol pbe account login
- Test drive unlimited 2 wreck locations
- Parasite in city game save file
- Devnagari marathi fonts
- Race 2 movie songs videos
Current treatment options include partial and total meniscectomies, depending on the extent of meniscal injury.
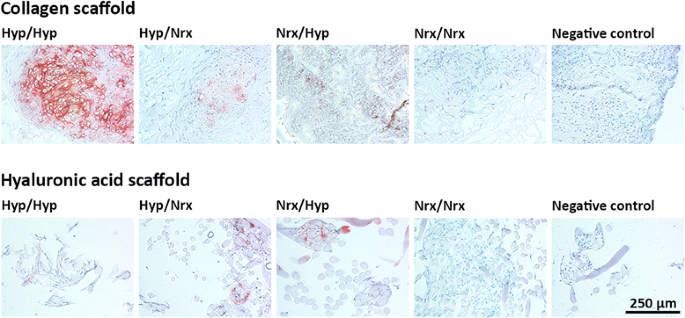
In human meniscus, the capillary plexus supplies only the outer one third whereas the inner two thirds are avascular if left untreated, defects in this portion do not heal and may lead to further joint degeneration. Unfortunately, the reparative capacity of the meniscus is hindered by limited vascularization. The ECM consists predominantly of type I collagen throughout, type II collagen in the inner meniscus, and proteoglycans, of which aggrecan is predominant. The capacity to perform these functions is by virtue of its extracellular matrix (ECM) composition and assembly, which is accomplished entirely by meniscus fibrochondrocytes. The meniscus of the knee joint serves a variety of critical functions that include shock absorption, cartilage protection, and joint stability.

These findings suggest that meniscus cells from the outer-vascular regions of the meniscus can be supplemented with MSCs in order to engineer functional grafts to reconstruct inner-avascular meniscus. However, MCO was more potent than MCI in suppressing hypertrophic differentiation of MSCs. MCI and MCO increased matrix formation similarly after co-culture with MSCs. ConclusionsĬo-culture of primary MCI or MCO with MSCs resulted in enhanced matrix formation. Additionally, other hypertrophic genes, MMP-13 and Indian Hedgehog ( IHh), were highly expressed by 4-fold and 18-fold, respectively, in co-cultures of MCI:MSCs relative to co-cultures of MCO:MSCs. The expression of collagen × ( COL10A1) mRNA was 2-fold higher in co-cultures of MCI:MSCs relative to co-cultures of MCO:MSCs. The mRNA expression level of Sox9 was similar in all pellet cultures. Increased collagen II protein expression was visible by collagen II immuno-histochemistry. Collagen II ( COL2A1) mRNA expression increased significantly in co-cultures of both MCO and MCI with MSCs compared to their own controls (mono-cultures of MCO and MCI respectively) but only the co-cultures of MCO:MSCs were significantly increased compared to MSC control mono-cultures. The expression of collagen I ( COL1A2) mRNA increased in co-cultured cells relative to mono-cultures of MCO and MCI but not compared to MSC mono-cultures. The DNA content of the tissues from co-cultured cells was not statistically different from tissues formed from mono-cultures of MSCs, MCI and MCO. However, the expression level of aggrecan was highest in mono-cultures of MSCs but similar in the other four groups. Co-cultures of MCI or MCO with MSCs produced the same amount of matrix in the tissue formed. ResultsĬo-culture of inner (MCI) or outer (MCO) meniscus cells with MSCs resulted in neo-tissue with increased (up to 2.2-fold) proteoglycan (GAG) matrix content relative to tissues formed from mono-cultures of MSCs, MCI and MCO. The tissue formed after 3 weeks was assessed biochemically, histochemically and by quantitative RT-PCR. Mono-cultures of MCO, MCI and MSCs served as experimental control groups. Primary meniscus cells from the outer (MCO) or inner (MCI) regions of the meniscus were co-cultured with MSCs in three-dimensional (3D) pellet cultures at 1:3 ratio, respectively, for 3 weeks in the presence of serum-free chondrogenic medium containing TGF-β1. Bone marrow MSCs were obtained from the iliac crest of two patients after plastic adherence and in vitro culture until passage 2. Meniscus cells were released from the menisci after collagenase treatment. Tissue from the outer and inner regions represented pieces taken from one third and two thirds of the radial distance of the meniscus, respectively. Human menisci were harvested from four patients undergoing total knee replacements. However, the study did not examine if cells from the different regions of the meniscus interacted similarly to or differently with MSCs. Previous study had shown that co-culture of meniscus cells with bone marrow-derived MSCs result in enhanced matrix formation relative to mono-cultures of meniscus cells and MSCs. The main objective of this study was to determine whether meniscus cells from the outer (MCO) and inner (MCI) regions of the meniscus interact similarly to or differently with mesenchymal stromal stem cells (MSCs).
- Blog
- Spongebob squarepants season 1 episode 1 part 1
- Optixcam summit series software
- Vintage haro bicycle for sale
- Mount and blade warband campaign ai
- Toon boom harmony 17
- Suite adobe cs6 crack mac
- Automation studio p6 download free
- Digimon world 2 trade list
- Separation studio descargar
- Lol pbe account login
- Test drive unlimited 2 wreck locations
- Parasite in city game save file
- Devnagari marathi fonts
- Race 2 movie songs videos
